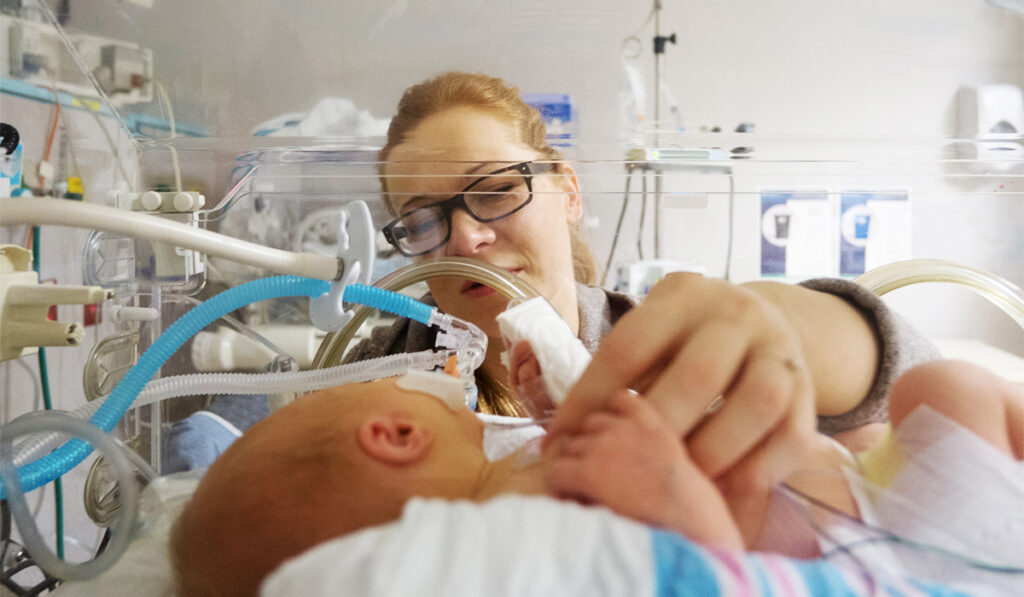
Improving rates of survival for infants born extremely preterm have resulted in greater demand for advanced respiratory therapies, along with a higher incidence of bronchopulmonary dysplasia (BPD) in preterm babies.
“Bronchopulmonary dysplasia is something that has been around since preterm babies were able to be successfully resuscitated,” said Dupree Hatch, M.D., medical director of the NICU at Monroe Carell. “Preterm babies are born at an immature place in their lung development, and many need respiratory support.”
Because of the potential impact on long-term lung health, BPD is one of the most frequent targets of neonatal quality improvement (QI) initiatives, and structured approaches of this type have been used successfully to implement better practices.
In 2018, multiple quality improvement teams at Monroe Carell Jr. Children’s Hospital at Vanderbilt began working to improve internal rates of BPD within the NICU, which serves as a regional referral center, by consolidating several previous QI initiatives into a comprehensive program.
“Even babies who don’t have bronchopulmonary dysplasia but were born preterm can have a higher incidence of lung problems later in life,” Hatch said. “Anything we can do in the NICU to lessen that burden is what the quality improvement program is about.”
“Anything we can do in the NICU to lessen that burden is what the quality improvement program is about.”
The team-based QI framework brings organization and support to the goal of improving respiratory outcomes in the unit. A five-year evaluation of the program, including future recommendations, was published in Clinics in Perinatology.
As a Level IV center, Vanderbilt’s NICU receives approximately 1,500 admissions annually, with 40 percent of cases arriving by transport.
“Our NICU takes care of infants born as early as 22, 23 and 24 weeks,” Hatch said. “BPD rates are inherently high in these infants due to the very early stage of lung development at which they are born and the intensive respiratory therapies they require to survive.
“But even in this population, BPD was higher than what we would have expected based on benchmarking data.”
Teams Divide and Conquer
BPD is a complex, multifactorial disease requiring multiple interventions for improvement, said Eva Dye, D.N.P., a neonatal ICU nurse practitioner and co-leader of the Vanderbilt project.
“It’s a difficult disease to affect because many aspects of nursing and medical care are interconnected and influence BPD outcomes,” Dye said.
“We each brought a different lens, which allowed us to better identify issues and practices that needed improvement,” Dye noted.
Hatch and Dye started constructing the QI program, a couple of foundational QI teams and several good initiatives had been approved, but most were one-off projects.
“We recognized that the way the program was organized wasn’t really helping to sustain improvement,” Dye said.
To establish priorities, a leadership team comprised of Hatch, Dye, Christa Sala, a respiratory therapist and a bedside nurse, Caitlin Pugh, engaged with senior hospital and unit leadership and frontline staff over a four-month period.
“We each brought a different lens, which allowed us to better identify issues and practices that needed improvement,” Dye noted.
Through these meetings and an extensive literature review, primary and secondary drivers were identified for the program and a NICU QI Dashboard established that was organized around the National Academy of Medicine’s six domains of health care quality.
Unit-based teams were assigned to address distinct aspects of care, including nutrition, infection prevention, mechanical ventilation, noninvasive ventilation, and antibiotic stewardship among others. A REDCap database was implemented to help teams share data across projects and drill down on specific priorities. This “microsystems” approach ensures that each team stays focused on its piece of the solution while coordinating with the overall program, Dye said.
Establishing Improvement Capacity
The Monroe Carell program benefited from existing QI program theory, and organizers are advocating use of existing, available methods, like the Model for Understanding Success in Quality (MUSIQ), to maximize the potential for quality improvement success.
Training is also essential, Hatch noted.
While he had undergone prior formal QI training, most team members had little structured exposure to QI principles. Both Hatch and Dye went through the I2S2 training program at Cincinnati Children’s Hospital, and others participated in Vanderbilt’s yearlong internal QI training program. Other team members attended day-long bootcamps.
“Having trained QI coaches embedded in each team and aligning our QI teams with external organizations such as the Tennessee Initiative for Perinatal Quality Care and the Vermont Oxford Network helps provide both internal and external motivation, which we think leads to sustainability of our results,” Hatch said.