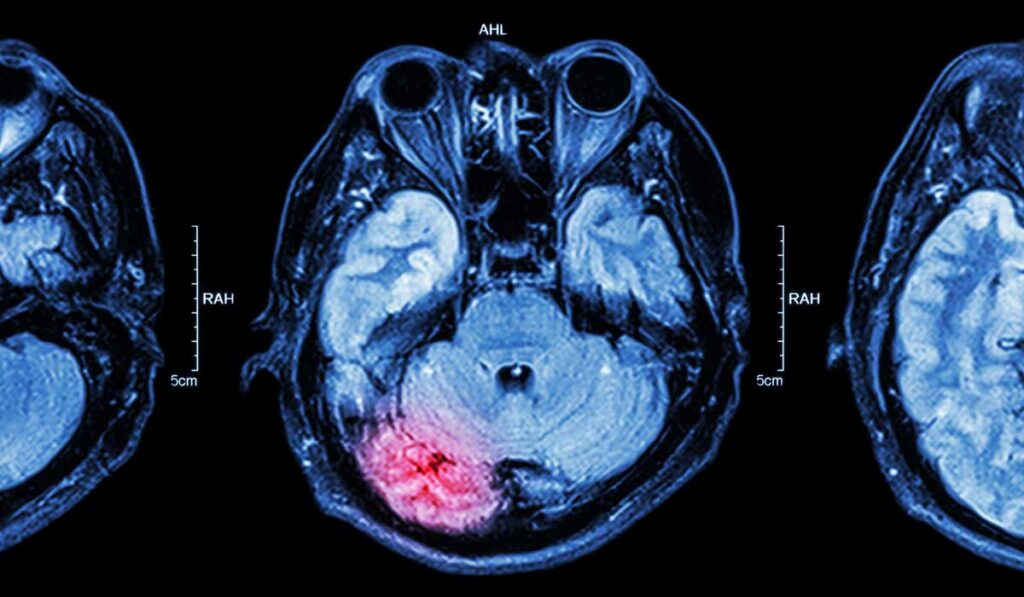
Football coaches whose advice to players is to “play through the headache” are not welcome in today’s football scene – at any level.
The sport is migrating to a more strategic game, where heavy physical contact is just one means of executing plays, not the primary objective.
As with most clubs for youth, high school and college athletes, the National Football League (NFL) has strengthened its rules to better protect all players on the field. Under the leadership of Allen Sills, M.D., chief medical officer for the NFL and founder of the Sports Concussion Center at Vanderbilt University Medical Center, the league continues to focus on how players can be protected from and treated for sport-related concussion and other injuries. His work has extended into enhancing evidence-based protocols around players who do become injured.
“We are committed to making the game as safe as possible, especially with respect to head injuries,” Sills said. “Every year we critically evaluate how we diagnose and treat concussions with some of the nation’s best epidemiologists and sports researchers. With their help and leadership, we have been able to affect several rule changes to reduce the incidence of concussion and head contact.”
Leadership from the Trenches
Sills, who founded the Sports Concussion Center in 2011, was a medical school mentor to Scott Zuckerman, M.D., an assistant professor of neurological surgery at Vanderbilt. Zuckerman serves as the center’s co-director. Along with neuropsychologist Douglas Terry, Ph.D., and six Vanderbilt sports medicine colleagues, he is as an unaffiliated neurotrauma consultant (UNC) for the National Football League during all Tennessee Titans home games. Their role is to make sure the Titans and visiting teams stay safe, and that every potential concussion is evaluated strictly according to the protocols of the NFL and the NFL Players Association.
“When it comes to concussion, the NFL has been completely revitalized since Allen Sills took over as CMO,” Zuckerman said. “The NFL is front and center on the international stage, really setting the gold standard for head injury management in all professional sports, including soccer, rugby and Australian rules football, among others.”
An active neurosurgeon, Sills has demonstrated consistent interest and passion throughout his career in caring for athletes.
“Every year we critically evaluate how we diagnose and treat concussions with some of the nation’s best epidemiologists and sports researchers.”
“You don’t just walk into a job with professional players,” Zuckerman said of his colleague. “Allen has taken care of athletes at all levels, which is really crucial. He has made his career working in the trenches, being on the sidelines of high school, college, and professional sporting events, working shoulder to shoulder with athletes, coaches and athletic trainers.”
Strategy for Success Affirmed
Sills’ immersion in concussion management inspired him to co-author a retrospective study of concussions in the NFL between 2015 and 2019 that measured the impact of concussion-reduction strategies implemented in 2018.
“The NFL is front and center on the international stage, really setting the gold standard for head injury management in all professional sports.”
A total of 1,302 concussions were identified over the five seasons, affecting 1004 players. Of these, 80 percent occurred during the games. A 23 percent reduction in concussions occurred over the course of the study, from an average of 231 in each of the first three seasons to an average of 177 for the final two. This affirmed the efficacy of the reduction strategies and established a baseline for measuring future gains.
The study concluded: “Complete and accurate characterization of when, how, and to whom these injuries occur can facilitate injury reduction efforts.”
No Magic Bullet
Training in concussion detection and management is ubiquitous throughout the league, from players to coaches to referees. Penalties for players who lead with their helmet and other violations linked with concussion are called with greater frequency today.
“Players, coaches and other staff are attuned to the fact that they’re going to be evaluated after a potential head injury,” Zuckerman said. “If it’s anything close to being dangerous or close to a concussion, they’re going to be asked to sit out, because it’s just the safest thing for them.”
“There is no single magic bullet to prevent all concussions.”
One major change to in-game NFL concussion evaluation was the creation of a blue medical tent on the sidelines of every game. “The sideline is a busy, congested, chaotic place,” Zuckerman said. “This helps remove the player and physician from a lot of the distraction and commotion, and we can do all our testing in a closed, standardized environment.”
The evaluations there are similar to the Sports Concussion Assessment Tool 5 (SCAT5), which primarily consists of the player answering orientation questions and undergoing vision, cognitive, and balance testing.
Under Sills’ guidance, three UNCs are assigned to every game, one posted on each of the sidelines and one in the booth. Two certified athletic trainers are positioned as spotters in the booth, watching every play from multiple angles to rule out concerning collisions.
New this year is the introduction of Hawk-Eye, an instant replay video system capable of capturing multiple angles of a play as well as a whole field perspective. “Many times, on-field medical professionals can’t see what’s going on under a pile of six to eight players. Having this Hawk-Eye system in the booth allows us to see any concerning signs such as motor incoordination, posturing, or loss of consciousness,” Zuckerman said.
“There is no single magic bullet to prevent all concussions,” he said. “They are inherent to any contact-oriented game. But if we can make the game as safe as possible by looking at all different areas of play both during practice and competition, then hopefully we can improve head injury safety at the NFL and all levels of play.”
Off-field Assessments
Every NFL team must also have a neuropsychologist working off the field on pre-season baseline cognitive evaluation, and then repeating those neurocognitive tests on players whose concussions are suspected or confirmed.
Katherine Gifford, Psy.D., an assistant professor of neurology at Vanderbilt, is the neuropsychological consultant for the Titans. One of her areas of research is developing tools for early detection of cognitive impairment.
“I’ve seen a lot of players over the years, including those who have trouble recovering or are noticing changes in cognition later in life. These advances in concussion identification, management, and monitoring are developed to increase player safety and health and are an important step in the right direction.”
Completing a neuropsychological assessment is part of the return-to-play protocol. It includes a 30-minute hybrid neurocognitive assessment that examines some of the most commonly affected areas after concussion – primarily memory and processing speed. Following an injury, athletes must return to their baseline cognitive skills to progress through the return-to-play.
“We have so many people on the field who are trained and expert at identifying hits that are potentially injury-causing, and this is head to toe,” Gifford said.
With the stricter, evidence-based concussion protocols and mandatory trainings on concussion becoming familiar in the NFL community, Gifford sees players increasingly on board with the precautions. “Players, trainers, and coaches all understand that these are the rules, and I find them very supportive of the process,” she said.