In the still-brief history of robotic-assisted procedures, this alternative to open or laparoscopic surgery is being recognized for improved outcomes for patients and superior ergonomics for the surgeon.
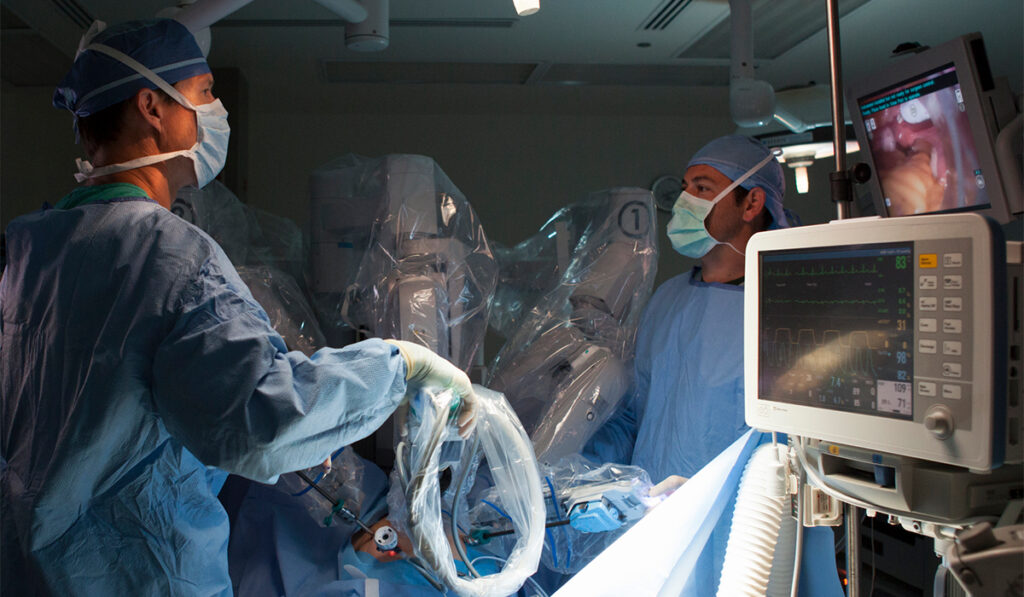
Kamran Idrees, M.D., chief of the Division of Surgical Oncology and Endocrine Surgery at Vanderbilt University Medical Center, launched the center’s robotics program for pancreatic and liver surgeries in 2019 and has since logged more than 80 such surgeries on patients from throughout the Southeast.
The agile “wrist” movement of the robot and improved visualization through high-definition, maneuverable cameras that allow access to major blood vessels – especially those underneath the pancreas – enable procedures that are not available through open or laparoscopic surgery, Idrees said.
His outcomes data are elevating confidence across the board for robotic assistance in surgeries from distal pancreatectomy to the highly complex total pancreatectomy with splenectomy.
“We do a majority of our procedures robotically now… and are finding not only significantly lower lengths-of-stay, but faster recoveries and avoidance of wound infections and other anatomical complications.”
A major plus is less need for hospitalization, as shown through the comparison of data on open and robotic pancreatectomy and splenectomy at Vanderbilt. Patients whose surgeons used robotic techniques are typically in the hospital only two to three days compared to more than seven days for those having open surgery, according to Idrees.
“We do a majority of our procedures robotically now, if technically feasible, and are finding not only significantly lower lengths-of-stay, but faster recoveries and greater avoidance of wound infections and other anatomical complications,” Idrees said. “Importantly, if the patient needs additional treatment such as chemotherapy, they can recover quickly and initiate this sooner.”
Malignancies Addressed
Of the various malignant conditions Idrees treats, the most common are pancreatic adenocarcinoma and pancreatic neuroendocrine tumors. The need for complicated partial or total organ resection in treating these tumors spotlights the distinct advantages of robotic surgery.
“We gradually started using robotics for carefully selected cancer patients with certain surgical needs, beginning with distal pancreatectomies,” he said. “Now, we are performing more complex pancreatic resections.”
The Whipple procedure (pancreaticoduodenectomy), in which the head of the pancreas is removed, is one of the most complex surgeries, requiring a high degree of planning due to the organ’s close proximity to multiple other organs and blood vessels. Idrees assisted Vanderbilt hepatobiliary surgeon Sekhar Padmanabhan, M.D., in their first robotic-assisted Whipple procedure in April of 2024.
Treatment of Premalignancies
Premalignant cystic lesions have a 10- to 40-percent potential of developing into pancreatic cancer over a lifetime. Vanderbilt operates a multidisciplinary cyst clinic to follow such patients, including those with intraductal papillary mucinous neoplasm (IPMN) or mucinous cystic neoplasm, Idrees said. Robotics are also used to resect these premalignant cysts, when warranted.
Padmanabhan has used robotics to perform the Puestow procedure for patients with chronic pancreatitis, in which the pancreatic duct is repositioned to drain into the small intestine.
In March of 2024, Idrees and Padmanabhan successfully performed the first robotic total pancreatectomy on a patient who had widespread premalignant changes from main duct IPMN. They used the DaVinci robot to remove the whole pancreas and spleen, part of the stomach and bile duct, and the duodenum. After the resection, two new delicate connections were created robotically from the small intestine to the stomach and from the small bowel to the bile duct.
Patients Move Forward Sooner
Instead of recovering from a 15-20 cm wound across the bottom of the ribcage over four to six weeks, patients undergoing robotic surgeries may be discharged the following day. Such a rapid recuperation from surgery has far-reaching benefits. Since the incisions are small, wound infection rates are extremely low, Idrees said. Incisional hernias, a not uncommon long-term sequala of open surgery, are a negligible risk.
“If a patient has a wound infection or they are weaker from open surgery, we have to delay chemotherapy and other therapies. If recovery is faster because of robotic surgery, these patients with cancers can generally move quickly to the next stage of their treatment, such as chemotherapy or chemoradiation therapy, and this has a profound impact on their overall survival,” Idrees said.