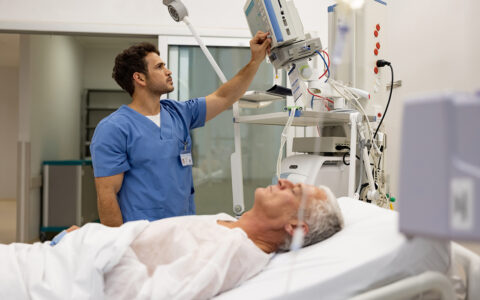
At Vanderbilt University Medical Center, a diverse team of researchers, providers, and stroke stakeholders is immersed in efforts to establish an innovative system of stroke care through a study called C3FIT (Coordinated, Collaborative, Comprehensive, Family-based, Integrated, Technology-enabled Care).
The randomized trial, led by national principal investigator Kenneth Gaines, M.D., and patient principal investigator and stroke survivor Barry Jackson, engages an Integrated Stroke Practice Unit featuring a multispecialty, mobile team to provide comprehensive follow-up care over the vulnerable first year following stroke.
Under a $15.7 million Patient-Centered Outcomes Research Institute grant, site principal investigator Jeri Braunlin, D.N.P., and national co-investigator and chief research scientist Patricia Commiskey, Dr.P.H., M.A., are working with Gaines to complete the seven-year study of C3FIT across 18 sites.
The researchers will compare the effectiveness of an Integrated Stroke Practice Model of care with a more traditional Comprehensive/Primary Stroke Center model.
“We have a disjointed system of care delivery in our country. The first year after stroke is a critically neglected time,” Gaines said.
“Besides recurrence risk, there are common secondary complications like clots in the leg, pneumonias and urinary tract infections. There is very high caregiver strain associated with that period of time. We are working to re-engineer this delivery system to improve outcomes, including patient and caregiver satisfaction.”
The study, which follows participants for 12 months after hospital discharge, is underway.
Cracks and Conflicts
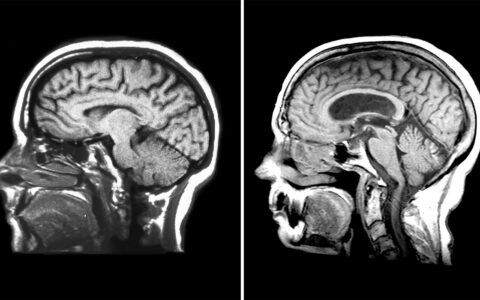
Recurrent stroke occurs in over 17 percent of patients with transient ischemic attacks and 18 percent with a non-disabling stroke in the first three months. After five years, nearly a third of survivors have had a stroke recurrence. The initial 12 months is a period where patients face significant disability, increased potential for recurrent stroke and re-hospitalization, and high rates of depression.
The body of research affirms what is intuitive: lack of a deliberate follow-up plan often leads to care that is poorly coordinated and a significant potential for error after discharge. In fact, Gaines says, only about a third of patients typically achieve their blood pressure and total cholesterol targets in the first year.
The urgency is clear from a sustainability standpoint as well, with significant stroke care costs incurred after the incident hospitalization.
C3FIT Features
C3FIT focuses on what Gaines and Commiskey call “the chronic nodes of care,” including recovery, prevention of recurrence and readmission, and risk factor management.
“We aren’t just dealing with stroke-related problems, but with the problems that surround a family that has experienced stroke.”
“Stroke recovery is largely about behavioral changes. Patients and their caregivers/family are under physical and emotional stress in the hospital, and often have difficulty recalling and implementing changes that could reduce stroke recurrence once they are discharged,” Commiskey said.
To help institute behavioral changes, the C3FIT arm of the study includes physicians, nurses, social workers, lay health educators, transitional navigators, and others – all with the goal of empowering patients to make changes in manageable pieces, building in success. One or more team member provides monthly visits to the home, often in-person, and this is augmented by giving the patient ready access both virtually and by phone to resources at the hospital.
“We aren’t just dealing with stroke-related problems, but with the problems that surround a family that has experienced stroke,” Braunlin said. “Through C3FIT, helping may mean finding extended physical or occupational therapy or free medications, helping with insurance paperwork or driving evaluations, transportation to their doctors’ appointments, and supporting them to obtain the supplies they need.”
Pilot as Springboard
Earlier, Gaines led a three-year Centers for Medicare and Medicaid Services Health Care Innovation Award study that enrolled 500 patient-caregiver dyads, with promising outcomes that provided a springboard for C3FIT. The researchers say these study results are to be published in late 2023.
“The beauty of the pilot is that we were able, during that period, to tweak things that didn’t work in real time, based on patient, caregiver, and other stakeholder feedback,” Commiskey said.
The study group used this feedback to refine their model.
“As one of the PIs in the C3FIT arm, I can say that alongside positive clinical indicators, evidence to date from both studies has highlighted the enthusiasm that patients and caregivers have for our mobile stroke teams,” Braunlin added. “This demonstrates that the stroke team is potentially fulfilling unmet needs for participants and their caregivers and it bodes well for patients’ successful reintegration into the community.”
Funds for the project were provided through the Patient-Centered Outcomes Research Institute.