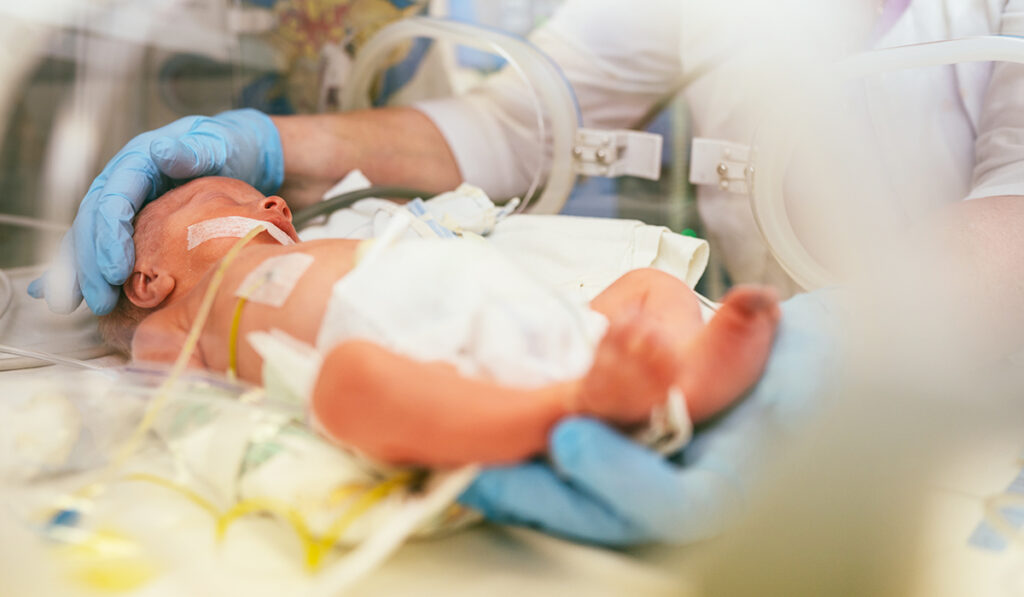
Genetics researchers are discovering that the same hypertensive genes that menace adults can confer an advantage in fragile babies.
Genetic epidemiologists at Vanderbilt University Medical Center have found an association between surviving babies with congenital heart disease (CHD) and a genetic predisposition toward adult hypertension.
The Circulation Research study by associate professor of medicine Todd Edwards, Ph.D., pediatric cardiologist Prince Kannankeril, M.D., and Ph.D. candidate Joseph Breeyear demonstrated a resoundingly strong and trending connection between alleles associated with high diastolic blood pressure (DBP) and babies with higher post-repair survival rates, shorter ICU stays and shorter total hospital days. This study follows other investigations showing a high blood pressure-related survival advantage in preterm babies.
“It made sense to us that if you were more susceptible to hypertension as an adult, you might respond better to vasopressors,” said first author Breeyear. “That’s exactly what we found: babies with a higher burden of blood pressure-increasing alleles needed less pharmacological help to achieve a stable blood pressure.”
While neonatal medical management precludes assessing blood pressure in these sick infants, the authors do not suspect these levels to be highly variable among the babies. Rather, they think the genes enable a high responsiveness to vasopressive medications or somehow reduce the need for vasopressors.
“It is remarkable to find a single factor that has an effect of this magnitude,” Edwards said. “Now, knowing a baby’s polygenic risk score for hypertension can prove extremely helpful in clinical and surgical preparation and post-op care.”
High-Powered Studies Deliver
Edwards leads studies of genetic variation associated with a range of conditions in the Million Veteran Program (MVP), a national program to study how genes, lifestyle and military exposures affect health and illness.
Using MVP data, Edwards and colleagues previously discovered associated with high blood pressure. In that study, Edwards and his team calculated polygenic risk scores by adding up the number of blood pressure-increasing alleles from a genome-wide association study of over 750,000 people. Essentially, the polygenic risk score is a continuous variable that shows an individual’s genetic predisposition towards high blood pressure.
Then they looked at genotyping data on 2,498 patients (infants through young adults) who had their first surgery for CHD at Monroe Carell Jr. Children’s Hospital at Vanderbilt, using blood and mucus samples Kannankeril collected between 2007 and 2020.
“One thing we had with this cohort of pediatric patients was medication use history – specifically vasopressors,” Kannankeril said. “So, our team applied a vasoactive inotropic score, which captures vasopressor treatment intensity, essentially giving us a gauge of how much was required to keep this individual stable.”
“Babies with higher polygenic risk scores needed less vasopressive medications to reach a stable blood pressure during and after surgery.”
They found that the reduction in mortality risk was linked to the interaction between genetic predilection of DBP hypertension risk and the dose of vasopressors. For each standard deviation increase in the DBP polygenic risk score, they estimated that the vasoactive inotropic score was reduced by about half.
“This affirmed that babies with higher polygenic risk scores needed less vasopressive medications to reach a stable blood pressure during and after surgery,” Kannankeril said.
Magnitude of Genetic Impact
From there, it was a small step to demonstrate that the reduced risk of mortality and ICU length of stay they found in these children was related to this interaction of blood pressure variants with the doses of vasopressors. This association showed remarkably strong alignment.
“For each standard deviation increase in DBP polygenic risk scores in our adjusted models, we estimated a 43 percent reduction in the odds of hospital mortality,” Breeyear said. “The greater the DBP alleles, the better the odds.”
Similarly, for every standard deviation increase, length of stay in the ICU was reduced by 2.41 days, a cost-savings of around $5,456 per patient.
Evolution for Survival, Condensed
The clinical implications of these findings are fairly straightforward. Knowing the DBP polygenic risk score and incorporating this with their vasoactive inotropic score could help guide decisions on how to titrate vasopressor treatment for hypotensive babies as a whole.
Further, though, Breeyear says the evidence of reduced hospital mortality in these patients motivates further exploration of adaptive processes underlying the high prevalence of hypertension in the global population.
“There is enough here to support a hypothesis that some of the increase we have seen in hypertension globally may be related to the survival effect of these genes,” he said. “Back when there was little that could be done medically to keep a premature infant alive – before all the interventions we do today – these infants depended on adequate innate vasopression to sustain their organ function. So those with more DBP alleles were the likely survivors.”
“Some of the increase we have seen in hypertension globally may be related to the survival effect of these genes.”
“While we have understood this association intuitively as clinicians, having the evidence that demonstrates such a clear and strong relationship opens doors to harnessing large genomic studies performed in adults to apply to pediatric populations of rare diseases,” Kannankeril added.