In many cases, Vanderbilt University Medical Center surgeons conduct lumbar spine procedures without opioid use, a practice that has led to positive outcomes. Yet, pain is a fact of life for many back surgery patients, immediately after their procedures and even months or years later.
Psychologist Carrie Brintz, Ph.D., is bringing her knowledge of psychological therapies to support lumbar spine surgery patients with better pain-related outcomes and increased odds of an opioid-free, higher quality of life.
Brintz, an assistant professor in the Department of Anesthesiology at Vanderbilt, is conducting a pilot study that combines components of mindfulness-based cognitive therapy (CBT) to create individualized telehealth sessions for patients at two to 12 weeks post-surgery.
“There is a large evidence base supporting CBT for pain management, both pre- and post-surgery,” Brintz said. “There are also solid studies showing that mindfulness-based interventions help with pain management, but little has been done to examine this with surgical patients. We wanted to fill this gap, and also test the impact when CBT and mindfulness meditation are combined.”
Brintz received seed money from the Osher Center for Integrative Health at Vanderbilt for the pilot. She will utilize funding from the NIH to refine the program and run a larger feasibility pilot before looking toward a multicenter randomized controlled trial.
Multiple Facets of Therapy
Chronic pain and disability persist for some lumbar spine surgery patients. With surgical rates rising and opioid prescribing rates starting to taper, the need to offer effective pain management options is more pressing than ever.
Brintz’s program targets pain perception, pain tolerance and quality of life. The design is based on psychological and neurobiological aspects of pain that mindfulness meditation and CBT have been shown to influence.
In the psychological realms, the program goals are to reduce patients’ tendency to catastrophize their pain, minimize fear avoidance, and increase patients’ threshold for pain, pain acceptance, self-efficacy, emotion regulation, positive affect and dispositional mindfulness.
The neurobiological goals are based on theory, tied into the still-emerging field of functional neuroimaging. Early studies show mindfulness meditation can cause neuroplastic changes in attentional control networks and appears to impact the function of the amygdala, which is associated with fear processing and negative emotions. Such therapy can reduce arousal – the fight or flight response – and drive other changes that may affect pain perception and tolerance.
Program Components
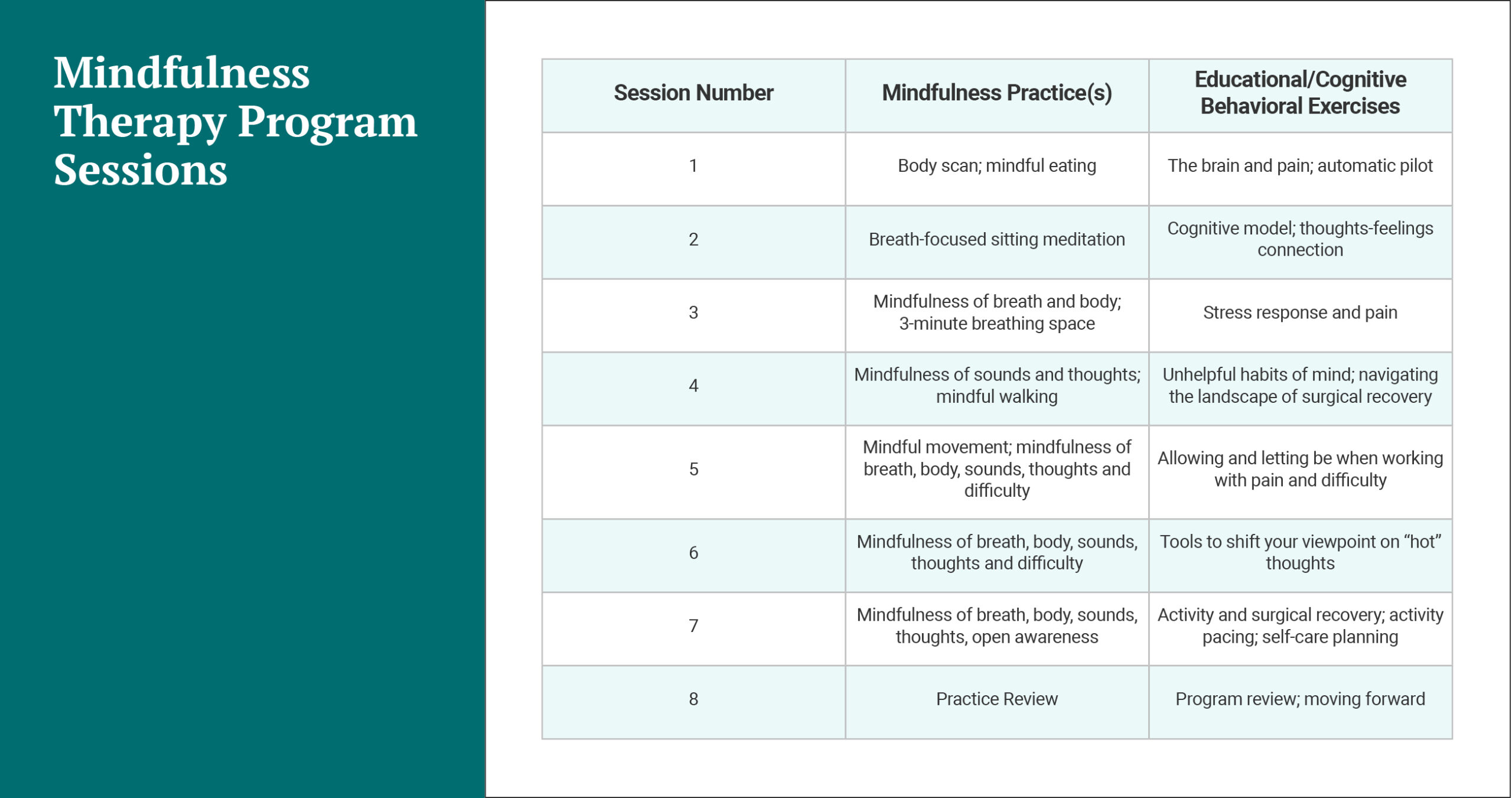
Nine patients completed the intervention, participating in eight weekly individual telemedicine therapy sessions beginning two to four weeks after surgery. Most participants reported practicing at home five to six days a week.
The pilot also incorporated a mindfulness movement component.
“Movement is critical to surgical recovery, but patients can be understandably fearful of resuming activity,” Brintz said. “This part of the therapy helps them to trust their body perceptions and venture out into walking and prescribed exercises.”
Shift in Importance of Pain
Through surveys and exit interviews, Brintz is investigating numerous variables: pain interference, opioid use, physical functioning, pain intensity, psychosocial variables, negative affect, dispositional mindfulness and pain-related benefits.
Key outcomes from the satisfaction survey included an overall high rating for physical and emotional well-being. Only three of the nine participants said the pain intensity decreased meaningfully due to the mindfulness intervention, but six said they were not nearly as bothered by the pain.
“I think these therapies help people start to tease apart the pain sensations that they’re having without all of the cascading reactions that can happen. They notice their pain, but they don’t react so intensely and with so much distress,” Brintz said.
While most participants said there was no difference in their need for pain medications because of the intervention, the standard postoperative treatment for these patients at Vanderbilt is designed to avoid pain spikes, while remaining opioid-free. Brintz says a large multicenter trial with a comparison intervention will be needed to better assess this program goal.
Larger Pilot on Tap
Such a high-powered multicenter trial is still a big step away. In preparation, Brintz and her team are designing a larger pilot with about 70 Vanderbilt patients, using the surveys and exit interview materials to refine the program and test its feasibility and acceptability among this population.
“We will also be looking at whether group or individual sessions are more effective,” Brintz said. “Group support can be really helpful from a social support standpoint, but with individual sessions you get that personal tailoring. We want to see where the data fall in that trade-off.”
