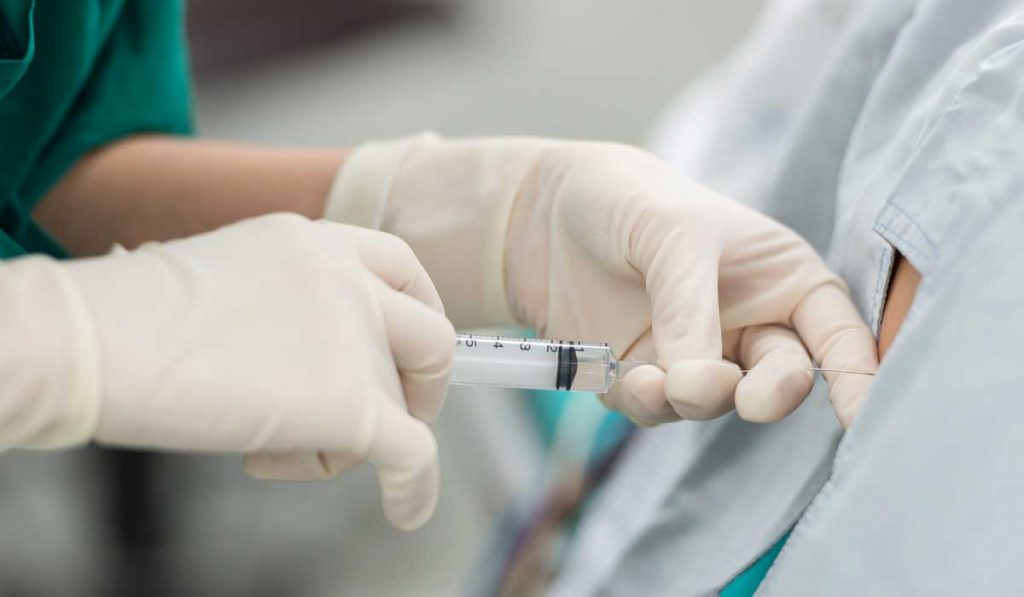
At Vanderbilt University Medical Center, leaders in spine physiatry and residency training are shortening the learning curve for interventional spine procedures through practice with cadavers. Residents have limited time to work on these interventional skills in the thick of their intense training programs, yet competency in some of these procedures is typically achieved after , says Aaron Yang, M.D., associate program director of the physical medicine and rehabilitation residency program at Vanderbilt.
“In clinical practice, the consequences of failing to reach full competency on these injections range from minor to catastrophic, and the residents understand these stakes,” Yang said. “A couple of years ago, our cadaver labs were basically used for locating anatomy. Now we are widely expanding the use of the enclosed cadaver as a practice field, giving them four to five times greater opportunities to practice on human tissue than they would have had in the past.”
The innovative approach is part of a larger trend in medical education to incorporate additional hands-on experiences for trainees. As Yang points out, gelatin and silicone simulators fall short of replicating human tissue. “They don’t give you the real sense of what it is to drive a needle through to the target. While cadavers are not live tissue, they are a close facsimile,” he said.
Meeting Growing Requirements, Demand
The American Academy of Physical Medicine and Rehabilitation guidelines now include competency in “therapeutic and diagnostic injection techniques” as a skill for residents. Yet in a recent survey of pain, spine and sports medicine fellowship program directors, 50 percent rated incoming physical medicine and rehabilitation-trained residents as below average in knowledge of and ability to perform interventional spine procedures.
“We are widely expanding the use of the enclosed cadaver as a practice field, giving them four to five times greater opportunities to practice.”
Yang led a 2019/2020 survey of graduating residents in U.S. physiatry programs, asking if they planned to do a fellowship after they graduated, and if so, what their subspecialty would be. From the 175 residents who responded, nearly 75 percent reported plans to do a fellowship and nearly 80 percent of them had matched into a pain, spine or sports medicine fellowship.
“Interventional spine procedures may play a major part in all three of those fellowships. We hope that cadaver practice for our trainees can help close the knowledge and skills gap,” Yang said.
COVID-19 Precipitated Personalized Training
Yang and colleagues started more frequent, personalized training about the time COVID-19 hit hard last spring. He says the pandemic forced them to be creative when they could not have the entire residency class in one room with the cadaver for a “watch-and-learn” session.
At Vanderbilt, an advisor and one or two residents work with a cadaver delivered with a C-arm, so the trainee can learn how to use fluoroscopy to guide injections. “In clinical practice, the radiation technologist obtains the images at the clinician’s direction, Yang said, “but if you have hands-on training in how to maneuver the fluoroscope, you’re more likely to understand the pictures you want.”
Enthusiasm Spurs Expanded Use
“After this individualized hands-on training, the residents came back saying it was one of the best educational experiences they have had so far – that they felt much more comfortable and confident after actually doing the procedures themselves,” Yang said. Yang says an informal survey of Vanderbilt’s own physiatry residents affirm this, rating the benefit to their education and training as an 8.8 out of 10.0. In fact, as more residents are benefitting from these practice opportunities, Yang says some are asking to use the lab to practice other interventions, such as ultrasound-guided procedures.
Vanderbilt is currently developing a formalized protocol for cadaver use in interventional spine training that can be shared across all residency programs. Said Yang, “I think the more time we spend in the cadaver lab, the more we can refine this protocol. We want to share this knowledge with other institutions.”