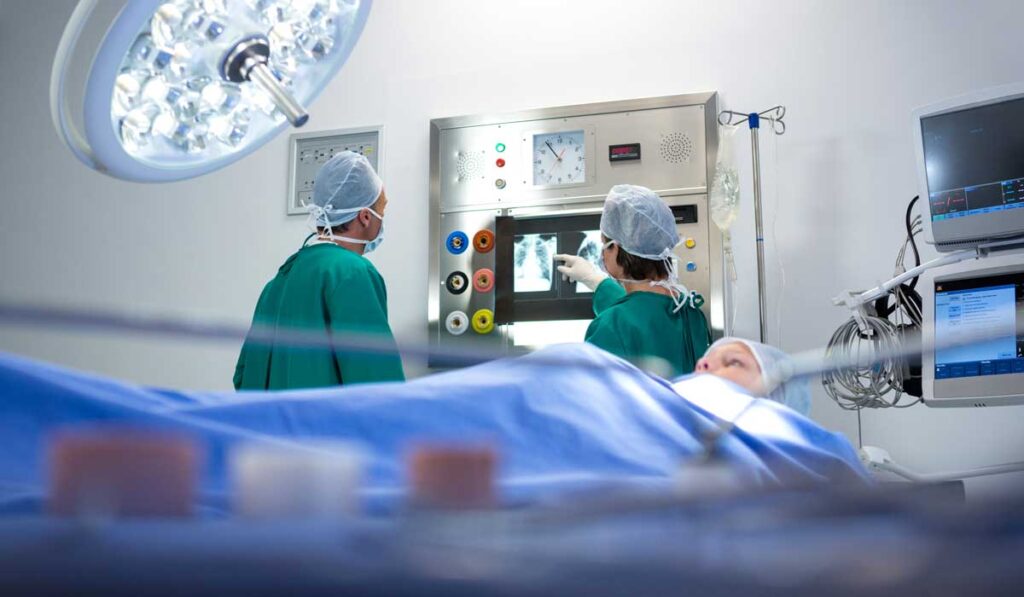
While experts advise against surgery for COVID-19 patients where possible, surprisingly little is known about risk of respiratory virus transmission in the operating room.
“No report to date has described the transmission of respiratory viruses, including SARS-CoV-2, in aerosolized surgical emissions during operations performed on patients of any age,” said Harold “Bo” Lovvorn III, M.D., a pediatric surgeon at Monroe Carell Jr. Children’s Hospital at Vanderbilt.
Lovvorn, together with Natasha Halasa, M.D., an associate professor of pediatrics at Vanderbilt, are co-principal investigators on a new grant from the Society of American Gastrointestinal and Endoscopic Surgeons to better understand SARS-CoV-2 transmission during surgery. The team is focusing their efforts on minimally invasive surgery in children.
Are Asymptomatic Children Vectors?
Non-emergent, minimally invasive surgeries have ramped up for children in recent months, say the researchers.
“Many children infected with SARS-CoV-2 are asymptomatic,” Halasa said. “Infected children could pose a significant risk of spreading the virus while undergoing routine procedures, like hernia repairs or laproscopic appendectomies.”
At present, the American College of Surgeons recommends personal protective equipment, including N95 respirators, for all surgical procedures that could generate aerosols.
Said Halasa, “Better determination of risk through studies like this one could help hospitals preserve adequate supplies.”
“Better determination of risk through studies like this one could help hospitals preserve adequate supplies.”
Looking for the Virus
The one-year study will first look for SARS-CoV-2 on nasal swabs collected from pediatric patients immediately after induction of general anesthesia. Any pediatric patient undergoing minimally invasive surgery at Vanderbilt will be eligible. Zaid Haddadin, M.D., postdoctoral research fellow in the Division of Pediatric Infectious Diseases at Vanderbilt, is in charge of recruitment.
Patient samples that rapid test positive for SARS-CoV-2 will be confirmed via PCR testing. During these patients’ procedures, the researchers will also sample condensation in the surgical port connected to the air evacuation system, and from the evacuation tubing, fluid collection chamber and filter. The environmental samples will also undergo more sensitive PCR testing to assess viral load in Halasa’s laboratory.
The researchers will determine whether SARS-CoV-2 can be detected in commercially available air evacuation systems after procedures in children who tested positive for the virus.
Measuring Virulence
Detecting SARS-CoV-2 is only part of the story though, Lovvorn said. He notes environment samples that test positive in Halasa’s laboratory will then head to Mark Denison, M.D., director of the Division of Infectious Diseases at Vanderbilt.
Denison’s coronavirus research team will then expose the samples to cell cultures. This critical step will determine if virus particles shed during surgery are truly infectious.
“Partnering with these outstanding virologists will maximize the chance to detect and understand the potential virulence of SARS-CoV-2 in aerosols emitted during minimally invasive surgery,” Lovvorn said.