A new report from the CDC examines trends in HPV-associated cancer incidence between 1999 and 2015 using data from cancer registries covering 97.8 percent of the U.S. population. In 1999 and 2015, respectively, 30,115 and 43,371 new cases of HPV-associated cancers were reported. There were slight decreases in cervical and vaginal cancer rates, but increases in oropharyngeal cancer, vulvar, and anal cancer rates. Penile cancer rates remained stable. The most common HPV-associated cancer in 2015 was oropharyngeal cancer (15,479 cases among men and 3,438 cases among women).
“The need for more effective prevention strategies remains critical,” said Ronald Alvarez, M.D., a gynecologic oncologist and chair of the Department of Obstetrics and Gynecology at Vanderbilt University Medical Center.
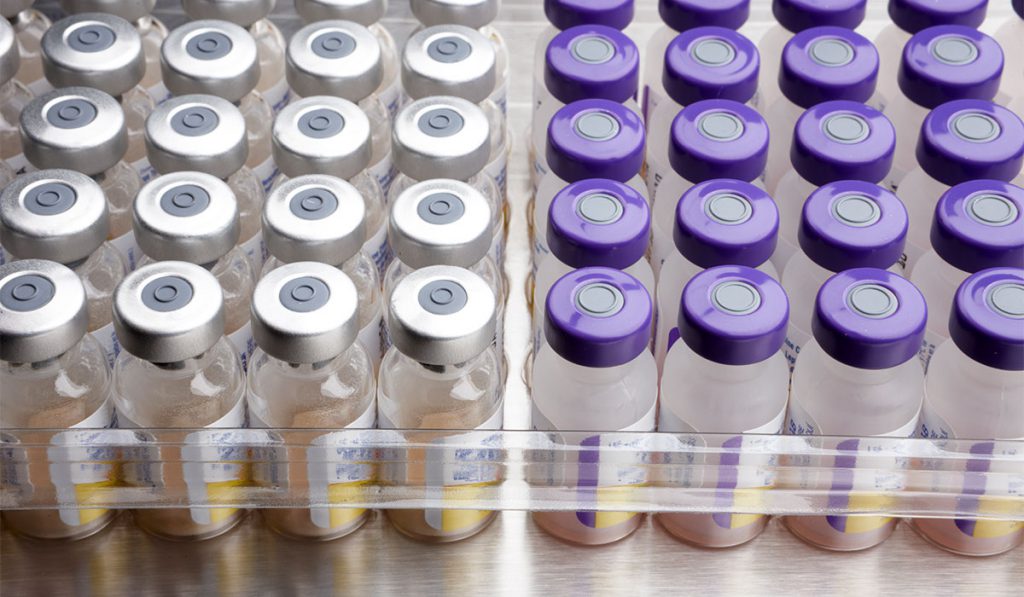
HPV Vaccination
“Every year, 14 million Americans become infected with HPV and 12,000 are diagnosed with cervical cancer.”
HPV vaccination for both girls and boys ages 9 to 26 has been recommended since 2006. Recently, the FDA expanded the indication for HPV vaccination with Gardasil 9 to include vaccination of women and men ages 27 to 45. The expanded indication is as a result of studies demonstrating Gardasil 9 to be at least 88 percent effective in the prevention of a combination of persistent HPV infection, genital warts, lower female genital tract precancers and cervical cancer from HPV types covered by the vaccine. The 9-valent vaccine targets oncologic types attributed to 73 percent of HPV-associated cancers, according to the CDC report.
“Every year, 14 million Americans become infected with HPV and 12,000 are diagnosed with cervical cancer,” Alvarez said. “HPV vaccination provides an opportunity to prevent more than 90 percent of these cancers, a phenomenon soon to be realized in countries like Australia that have school-based HPV vaccination policies.”
Cervical Cancer Screening
The CDC report attributes decreased cervical cancer rates between 1999 and 2015 to increased cervical cancer screening. Cervical cancer screening remains an important risk prevention strategy. Screening can detect precancerous cervical lesions that can be effectively treated before cancer develops.
The US Preventative Task Force (USPFT) recently released new recommendations for cervical cancer screening. Specifically, screening should not be performed before the age of 21. Between ages 21 and 29, the USPTF recommends cervical cytology be performed every three years. Between the ages of 30 and 65, the USPTF recommends high-risk HPV testing alone or in combination with cervical cytology every five years. Cervical cancer screening is not recommended for women beyond age 65 with no prior history of cervical dysplasia or for women who have had a hysterectomy for benign indications.
HPV Infection and Associated Cancers Symposium
After a successful 2018 symposium, HPV ACTIVE, a Vanderbilt-funded HPV-Associated Cancer Consortium, is sponsoring its second annual HPV Infection and Associated Cancers Symposium on March 1, 2019. Topics will include new and developing cervical cancer screening and HPV vaccination strategies. Registration information is available through the Department of Obstetrics and Gynecology.