Over 42 percent of Americans have obesity, the highest rate ever for the condition in the United States, according to recent CDC reports.
Comorbidities such as type 2 diabetes, hypertension, and dyslipidemia – along with extensive quality-of-life issues – often emerge early in patients with obesity.
Thus, bariatric surgeons are including younger patients in the cohort considered as candidates for metabolic surgery – bariatric surgery with the specific intent to treat diabetes and other metabolic disease. Their goal is to address the problems before they turn into serious, lifelong health issues.
“A big part of the decision to offer bariatric surgery to younger patients is to treat weight-related conditions earlier in their course, or prevent them from developing entirely,” said Christopher Menzel, M.D., a surgeon at the Vanderbilt Weight Loss Center and medical director of the bariatric surgery program at Vanderbilt Wilson County Hospital.
Younger surgery patients in their 20s and 30s are now being joined by a subset of teens.
“Many of the obesity-related conditions, such as diabetes, polycystic ovary syndrome, and sleep apnea, among others, greatly impact patients’ lives in those formative years, which can change the trajectory of their mental, physical and emotional health,” Menzel explained.
Guidelines Expand
In October 2022, two of the world’s leading authorities on bariatric and metabolic surgery – the American Society for Metabolic and Bariatric Surgery and the International Federation for the Surgery of Obesity and Metabolic Disorders – issued new evidence-based clinical guidelines for weight-loss surgery for the first time in 30 years.
The guidelines call for expanded use of metabolic surgery, stating “metabolic and bariatric surgery is currently the most effective evidence-based treatment for obesity across all BMI classes” and that it may be considered in “appropriately selected children and adolescents.”
The guidelines also state that weight-loss surgery should be considered starting at a BMI of 30 for people without metabolic disease who do not achieve substantial or durable weight loss or obesity disease-related improvement using nonsurgical methods.
Non-Surgical Weight Loss Limits
Obesity itself is a complex metabolic issue, Menzel explained. Individuals with high BMIs are often unable to achieve substantial or durable weight loss using nonsurgical methods because of metabolic adaptation – when the body slows metabolism to avoid excessive weight loss.
“It’s a survival mechanism. In times of starvation, our metabolism slows to allow us to survive. The problem in today’s day and age is resources are plentiful in many countries, so this mechanism is pathologic for purposes of weight loss,” Menzel said.
The surgeon said he began pondering questions about weight loss and metabolism even before he became an M.D.
“Prior to medical school, I worked as a personal fitness trainer and nutritionist,” he said. “People I worked with would lose weight over a period of time, but eventually they would hit a plateau – whether it be at a loss of 20 pounds or 100 pounds – and couldn’t lose any more weight. I saw the struggles first-hand, despite meal planning, calorie counting and intense exercise. That’s part of where my passion to become a bariatric surgeon comes from.”
Access and Advancements
“Surgical procedures we do can effectively reset the metabolism and help patients overcome this metabolic adaptation-related plateau to achieve tremendous, durable weight loss,” Menzel said.
Menzel supports the new guidelines that increase weight-loss surgery access, especially for younger people. He hopes the procedure will no longer seem like a last resort.
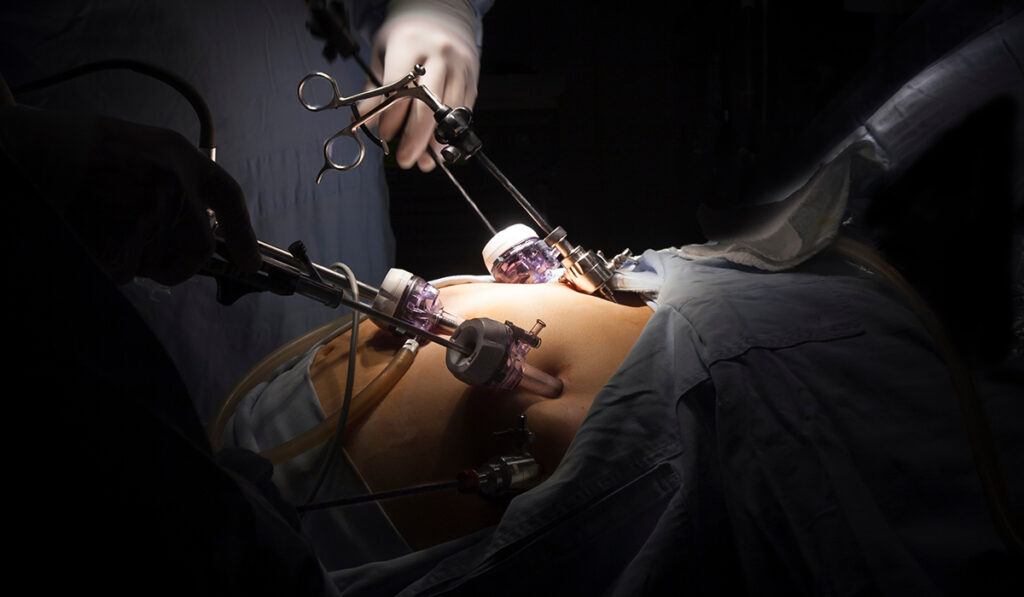
Older surgical techniques have been replaced by safer and more effective ones, with laparoscopic procedures, sleeve gastrectomy, and Roux-en-Y Gastric Bypass, now accounting for the majority of operations performed worldwide, Menzel said.
“Most of my patients who underwent the procedure in their 30s and 40s say, ‘I wish I had done this 10 years ago.’
“By undergoing a procedure that’s safe and takes about an hour or so, people really change the trajectory of their lives.”