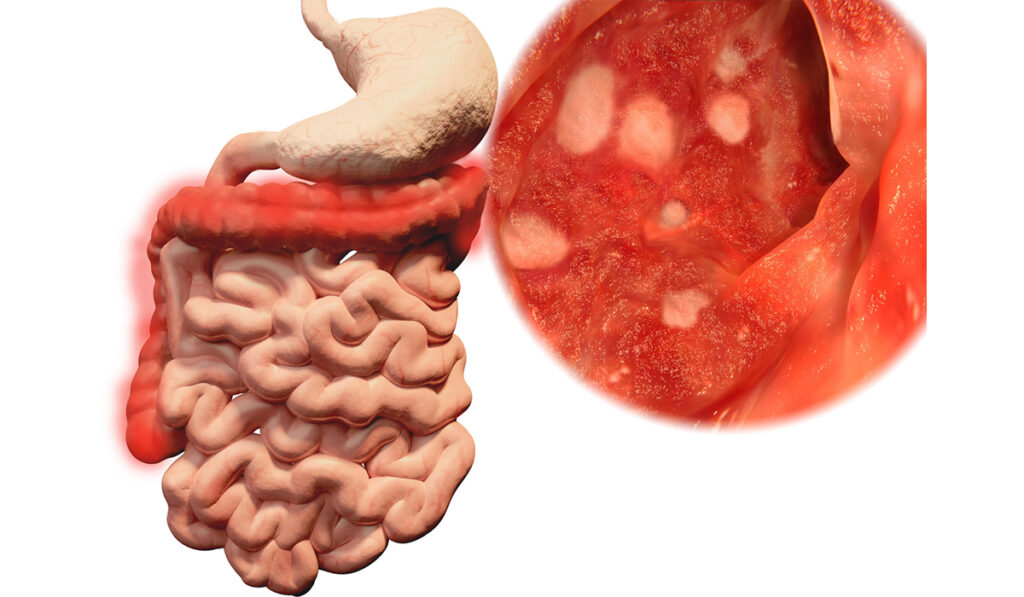
Patients with ulcerative colitis and other inflammatory diseases of the gastrointestinal tract have about an 18 percent chance of developing colorectal cancer over the course of 30 years.
Chronic inflammation has been identified as a primary culprit in the initiation and progression of many cancers, and disruption of the transforming growth factor-β (TGF-β) pathway is often implicated as a key factor.
Researchers at Vanderbilt University Medical Center have been working to discover how this pathway regulates the development of colorectal cancers. Through two papers, published in 2018 and 2022, R. Daniel Beauchamp, M.D., the J.C. Foshee Distinguished Professor of Surgery and co-leader of the Gastrointestinal Cancer Research Program, and Anna Means, Ph.D., a professor of surgery and cell and developmental biology, explored characteristics of the TGF-β pathway.
They and their colleagues determined that cellular loss of SMAD4, a transcription factor that propagates the signals downstream of TGF-β, contributes to pro-tumorigenic inflammation in gastrointestinal and pancreatic tumors. Specifically, they elucidated the link between loss of SMAD4 and induction of the chemokine CCL20 and its receptor, CCR6, in promoting this response.
“The goal is to interrupt the complex, multicellular events that spur malignant growth in the colon,” Beauchamp said. “We’ve known for quite some time that loss of SMADs within the TGF-β pathway interrupts the signaling from the TGF-β receptors to the nucleus. Now, our research demonstrates that loss of SMAD4 in the colon epithelium contributes to colorectal cancer risk by increasing inflammation, in part by enhancing CCL20 expression and chemoattraction of CCR6-positive immune cells.”
Beauchamp and Means also see CCL20 and its unique CCR6 receptor as potentially attractive targets for therapy.
“We believe disruption of the TGF-β pathway is critical in inflammation and cancer development,” Means said. “We are actively pursuing the receptor CCR6 as a potential target for colorectal cancer prevention in patients with ulcerative colitis and as a means of restricting colorectal tumor growth.”
SMAD4 as Mediator
To maintain homeostasis, the colon must attract immune cells when inflammation is required to repair damage and prevent invasion by harmful microbes. Too much inflammation, however, is associated with chronic ulcerative colitis and other inflammatory conditions of the gastrointestinal tract.
“The goal is to interrupt the complex, multicellular events that spur malignant growth in the colon.”
The SMAD signaling pathway is the central mediator of TGF-β signaling, operating downstream of its superfamily of ligands. It propagates the great majority of TGF-β biological responses – including proliferation, differentiation and apoptosis – in many different organ systems. SMAD4 is important because it is the common intracellular signaling molecule between all the different signaling inputs to the SMAD/TGF-β pathway.
Beauchamp explains that the SMAD4 gene is often mutated in pancreatic and colon cancers, but the consequences are not completely understood. Their studies have shown that loss of Smad4 in normal colon epithelial cells of mice increases the expression of chemokines that attract T cells, B cells, neutrophils, and monocytes, suggesting a range of inflammatory mediation.
“Restoring expression of tumor suppressor genes, including SMAD4, in an intact organism is not currently feasible. Better targets for therapy may be secreted regulatory proteins and their receptors that may be turned on because that tumor suppressor pathway is lost,” Beauchamp said.
SMAD4 and CCR6 Inhibition
In the new study, published in Gastroenterology, Means and Beauchamp used dextran sodium sulfate to drive chronic colitis in mice. When this inflammation was induced with the Smad4 gene selectively missing in intestinal epithelial cells, the mice developed cancer, and the resulting tumors strongly resembled human colitis–associated carcinoma.
“We are actively pursuing the receptor CCR6 as a potential target for colorectal cancer prevention in patients with ulcerative colitis and as a means of restricting colorectal tumor growth.”
However, additional loss of the Ccr6 gene markedly reduced the incidence of colitis-associated tumors.
In their human tissue studies, they found loss of SMAD4 in approximately half of human colitis–associated carcinoma samples as compared with about 20 percent of sporadic colorectal carcinomas, consistent with a strong link between loss of TGF-β activity and pro-tumorigenic inflammation.
Clinical Implications Now and in the Future
The researchers say more studies are needed to gather broad data that may affirm their findings before moving toward the clinic.
“We need to understand how CCR6 is working within the immune system and what exactly are the risks of side effects, such as potential unanticipated effects on inflammation,” Means said.
Some diagnostic applications of these studies may come sooner. For patients with ulcerative colitis, the screening potential is clear. Additionally, SMAD4 is lost in many other tumors where its absence may play similar roles. Means and Beauchamp are particularly interested in testing this in pancreatic cancer.