Harnessing the power of magnetic fields for medicine first changed the landscape in imaging, and it has since expanded therapeutic options for a range of neurological conditions. Now, a new device developed at Vanderbilt University Medical Center engages magnets to improve colonoscopy and upper endoscopy procedures.
Gastroenterologist Keith L. Obstein, M.D., a professor of medicine at Vanderbilt, and Pietro Valdastri, Ph.D., chair in robotics and autonomous systems at the University of Leeds, partnered with Vanderbilt’s STORM Lab to develop the remotely operated magnet-based technology. Its primary advantages flow from the ability of the operator to pull the tip of the endoscope through the intestinal tract using magnetic coupling and a robotic arm.
“Providers who perform endoscopic procedures know the physical strain that can be involved with repeat exams, as well as the threat of perforating tissues as you move a standard colonoscope forward,” Obstein said. “This coupled magnet platform gently pulls the device from the tip, so the endoscope moves smoothly through the colon, exerting much lower force on the bowel wall. We call it ‘front-wheel versus rear-wheel drive.’”
The magnetic flexible endoscope platform was first formally introduced in a 2018 paper published in Gastroenterology. Since then, Obstein and colleagues have improved on the technology and are now planning first-in-human trials for late 2022.
Autonomous Magnetic Endoscopy
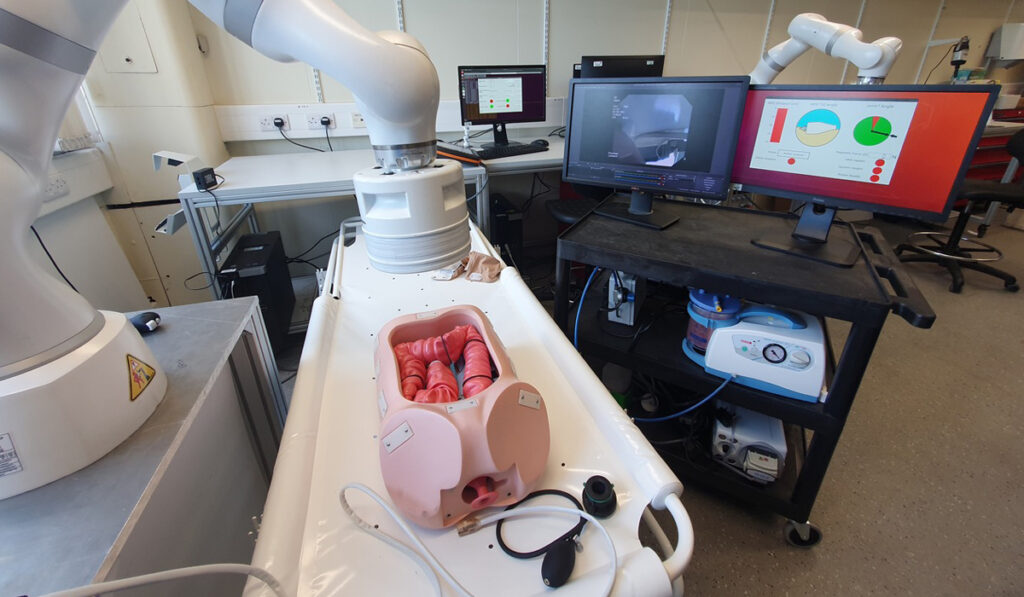
The magnetic flexible endoscope platform consists of control software, a magnet-embedded custom endoscope, and a serial robot, external to the patient, that actuates a permanent magnet mounted at the end of the arm. The magnet couples with the endoscope to provide proprioceptive sensing and guidance.
“The user can sit either near the patient, or potentially hundreds of miles away, and use a joystick to drive the robot, which autonomously guides the endoscope along the path of the lumen,” Obstein said. “It’s a closed-loop system, with the user making simple decisions like ‘turn left’ or ‘turn right’ or ‘look up.’”
The tip has a therapeutic channel for passage of surgical tools commonly used in standard colonoscopy, and can retroflex anywhere in the colon to perform therapy – a capability that is not possible with a standard endoscope.

“Previous endoscope advances have placed more cameras on the tip for looking back, but this made the endoscope larger and more difficult to maneuver,” Obstein said. “You could see the lesion behind you, but without retroflexion ability, it was extremely challenging to perform therapy.”
“This coupled magnet platform gently pulls the device from the tip, so the endoscope moves smoothly through the colon. We call it ‘front-wheel versus rear-wheel drive.’”
Happier Practitioners
Obstein says the ergonomic benefits of this system cannot be overstated. Shoulder and repetitive wrist, finger, thumb, and neck injuries famously menace endoscopists, who often are required to stand for hours on end while manipulating bulky wheels on the endoscope and twist the instrument shaft while looking up at a monitor. Instead, the operator of the magnetic flexible endoscope may be seated directly facing the monitor, joystick in hand.
Even better, he says, the team is developing a touchscreen interface allowing the operator to tap to indicate movement and desired direction.
“As long as you have a trained technician with the patient, there could be a remote gastroenterologist managing the colonoscopy.”
Happier Patients
Patients also stand to benefit from greater comfort, less risk of tissue perforation, and avoidance of sedation with the robotic platform, which would permit patients to drive themselves to and from their appointment.
With early-onset colorectal cancer on the rise, and the recommended screening age recently dropping from 50 to 45, Obstein believes these improvements will encourage more patients to get screened at younger ages and have suspicious GI symptoms checked out sooner.
Meeting Growing Demand
Any demand for increased testing calls attention to the short supply of gastroenterologists. In the future, however, adoption of the new robotic platform may enable endoscopies to be carried out by a primary care physician or general surgeon, a boon to rural and remote areas where specialized gastroenterologists are scarce.
“As long as you have a trained technician with the patient, there could be a remote gastroenterologist managing the colonoscopy. I can even foresee one clinician supervising multiple procedures at one time, similar to an anesthesiologist supervising three or four operating rooms run by CRNAs [certified registered nurse anesthetists],” Obstein said.
The team is now poised to transition from phantom, porcine, and cadaver testing to human trials to demonstrate that they can drive the platform from rectum to cecum and do so safely.
“Next steps will be to look at patient comfort and gather comparative data on lesion detection and resection,” Obstein said. “We have seen firsthand the many advantages of this system and anticipate a huge benefit for patients.”