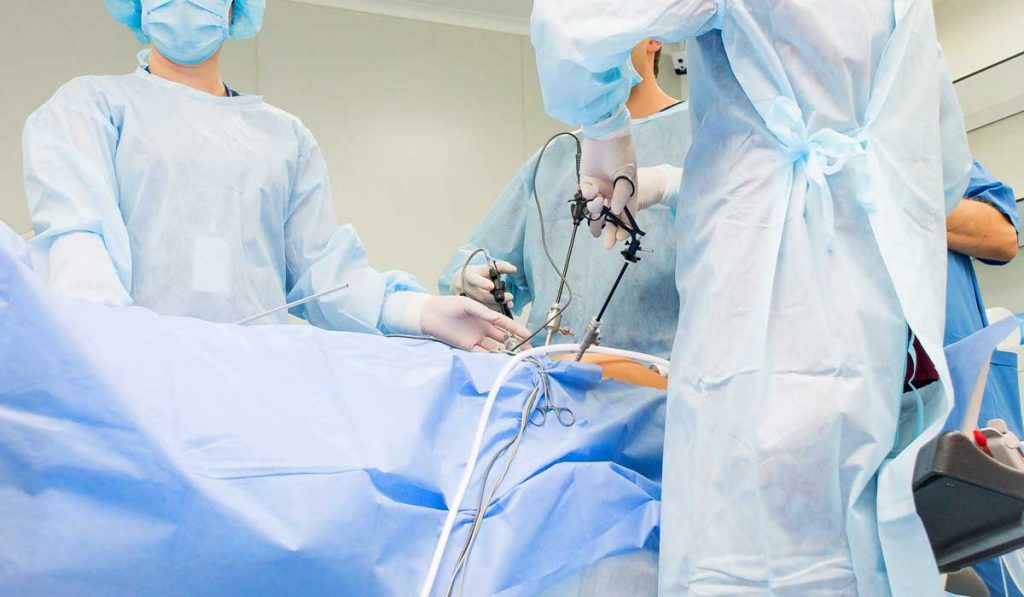
Despite a relatively static incidence rate of colorectal cancer in the U.S., the number and complexity of procedures that reduce morbidity and mortality are expanding. Responding to these opportunities, Vanderbilt University Medical Center is launching a new fellowship program in colorectal surgery.
The Colon and Rectal Surgery Fellowship will be housed in the Division of General Surgery. Molly Ford, M.D., a colorectal surgeon, will serve as program director. It is the second fellowship within the division, alongside the decades-old Advanced GI Minimally Invasive Surgery/Bariatric Fellowship.
“We’re all very excited because this has been years in the works; a lot of the excitement comes from being able to impart our clinical knowledge to the next generation – people who can carry the work forward,” Ford said.
Components of the Colorectal Surgery Fellowship
This one-year, accredited fellowship will be taught by one part-time and seven full-time faculty members. In addition to clinical education, fellows will have access to a simulation laboratory that includes a wet and dry lab, laparoscopic and endoscopic simulators, and state-of the-art da Vinci systems for robotic surgery simulations.
Training will span colonoscopy, abdominal and pelvic surgery, anorectal surgery, clinical management and inpatient care. It will include treatment of a wide variety of colorectal diseases and instruction on open, laparoscopic and robotic techniques.
“We’re all very excited because this has been years in the works; a lot of the excitement comes from being able to impart our clinical knowledge to the next generation – people who can carry the work forward.”
“At Vanderbilt, we get referrals for a lot of rare disease processes. We are able to treat a large percentage of these cases through minimally invasive robotic or laparoscopic procedures,” Ford said. Postoperative inpatient care utilizing Vanderbilt’s enhanced recovery pathway, which has significantly reduced complication rates since its inception in 2017, will also be a focus.
A Sister Program
Vanderbilt’s Advanced GI MIS fellowship was established in 1995 and grew to include a bariatric component in the early 2000s. Its program director, Brandon Williams, M.D., a minimally invasive bariatric surgeon, says Vanderbilt has always been a leader in minimally invasive foregut, bariatric, and hernia surgery.
“We perform a high volume of laparoscopic Roux-en-Y gastric bypass as well as complex revisional bariatric and foregut operations,” Williams said. “We put a strong emphasis on teaching free-needle laparoscopic suturing, which is more challenging to master, but develops a highly versatile capability. Our fellows gain a truly advanced skill set, with the ability to safely and confidently perform challenging operations.”
New Options for Complex Diseases
With the high prevalence of severe obesity, Williams says he and his colleagues would like to see a dramatic increase in the use of bariatric surgery.
“Much as with the colorectal program, our enhanced recovery pathway has greatly improved the patient experience for our bariatric patients. We train our fellows not just how to perform operations with expertise, but also how to deliver an exceptional level of patient care throughout the entire perioperative process,” Williams said. Fellows also devote time to research projects, focusing on quality improvement and outcomes following minimally invasive foregut and bariatric surgery.
In foregut surgery, the MIS fellows master the traditional laparoscopic treatment of gastroesophageal reflux, paraesophageal hernias and achalasia, with operations such as Nissen fundoplication and Heller myotomy. They also learn novel, emerging laparoscopic and endoscopic techniques, including magnetic sphincter augmentation and peroral endoscopic myotomy.
While foregut and bariatric surgery have long been the main strengths of the Vanderbilt Advanced GI MIS/Bariatric fellowship, the addition of new faculty in recent years has broadened its scope, adding a strong robotic hernia repair component, including extended totally extraperitoneal repair (eTEP).
For the Love of Teaching
Vanderbilt’s fellowship portfolio offers fellows a powerful bench of mentors. “The reason most of us are at Vanderbilt is that we like to teach,” Ford said. “Working at an academic institution, we all have a vested interest in education – more than is typically found in the private practice model.”
Williams adds, “A huge strength is that we have a diversity of faculty members on our team. Many MIS fellowships are more like an apprenticeship, but at Vanderbilt more than half a dozen surgeons contribute to the experience of our MIS fellow. If you can get good, quality training and mentoring from multiple surgeons instead of one or two, it’s all the better!”