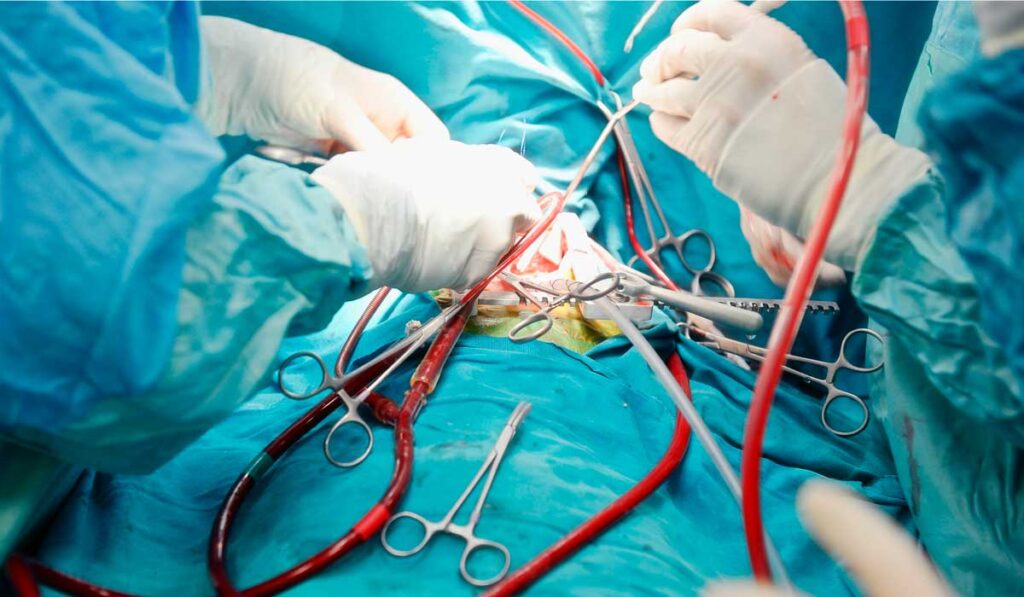
Modern medicine doesn’t have a tonic for lovesick hearts, but an astounding number of people get heart transplantations in Nashville, Tenn. The path to transplantation is as much of an emotional rollercoaster as an exhibit of advances, courage and despair.
The Vanderbilt Transplant Center was featured this fall in a three-part documentary on discovery+ called “Last Chance Transplant.” The number of people who have received organ transplants is growing, and there’s a chance you know someone.
This episode spotlights heart transplants, for which the demand outpaces the supply. That imbalance is a rallying cry for the transplant team at VUMC to find ways to get more people with broken hearts on the path to home.
Ashish Shah, MD, Professor of Cardiac Surgery, Alfred Blalock Endowed Directorship in Cardiac Surgery, and Chair of the Department of Cardiac Surgery, leads a team that is discovering innovative ways to fix failing hearts.
And as of 2020 surgeries, the VUMC team performed the most heart transplants of any center, anywhere. It averages out to about one every three days. In August 2020 they performed four transplants in 48 hours.
Shah and his peers are driven by the desperation and courage of their patients, who are willing to go to extraordinary lengths to live.
“The one thing that I get to do that no one gets to see is heart surgery and what the human heart looks like in all its various functions and dysfunctions. Some of these things are really—they’re just miraculous and amazing. I mean, I love heart surgery. I think everything about the heart is extraordinary and all the things that we’re learning about is amazing,” said Shah.
‘Why haven’t I been given that opportunity?’
There is a finite number of hearts available to transplant – it’s a natural constraint stemming directly from the limited number of people who are willing to be or can be donors.
Meanwhile, there’s of course constant, rapid advancement in all sectors of medicine. Those dual realities put Kelly Schlendorf, MD, MHS, Assistant Professor of Medicine, Director, Heart Failure and Transplant, and Medical Director, Adult Heart Transplant Program, on the path to a creative, collaborative method.
The team found patients were ready and willing to receive hearts infected with Hepatitis C since recently approved therapeutics can cure the virus. Using Hep-C infected hearts expanded the depth of the donor pool.
“I often joke saying that when I went into cardiology, I never thought I would realize or learn quite as much as I have about, about hepatology and hepatitis C specifically,” said Schlendorf. “When we started the hepatitis C effort, we as a program made a conscious decision that we were going only going to offer the opportunity to consider these donors to a select number of patients on our wait list. Specifically, patients who we felt like had a high likelihood of potentially dying on the wait list.”
Then 18 months into the program, the option opened to all active candidates on the wait list. It was motivated, in part, by the promising results.
And the team was motivated by clamor from patients who learned about it from the heart transplant communities on social media.
“Pre-transplant and post-transplant talk to one another via any number of social media platforms. And so interestingly enough, patients were coming to us and saying, ‘I understand so-and-so has been given this opportunity to consider a heart from a hepatitis C infected donor. Why haven’t I been given that opportunity,’” said Schlendorf. “So as a program we talked about this and ultimately decided that so long as we educate patients and their caregivers about the potential risks and benefits of this option, about what we know and what we don’t know about this option — that the decision really should be theirs and not ours.”
‘There’s a lot of negotiating’
The path to transplantation, and recovery is as much of an emotional rollercoaster as a test of physical and medicinal endurance. The psychological toll impacts a patient as well as their family and friends. It’s fraught with emotion, burdens, fatigue and often misalignment between reality and expectation.
Lesley Omary, MD, assistant professor of clinical psychiatry and behavioral sciences as well as director of the Transplant Psychiatry Service, works with patients undergoing this lifechanging procedure pre-transplant as well as follow-ups for situations that arise post-transplant.
“We do see actually some interesting conflict sometimes [with] how this gets managed and people’s family. We try to help people navigate that because sometimes a patient has had their transplant and they’re doing well, but they’re not a hundred percent back to normal,” said Omary. “So they still may need some assistance at home. But the family member is exhausted. Caregivers are exhausted and they’re like, ‘I can’t do anymore. You’ve had your transplant. It’s time for you to get back to, you know, helping out.’ But maybe they’re not there yet in their recovery. So there’s a lot of back and forth. There’s a lot of negotiating and we do help with that sort of issue.
‘How do you resuscitate these hearts and recondition them?’
Transplant surgeons along with biomedical engineering colleagues, and many others, are constantly flexing the boundaries of what’s possible.
It’s not lost on Shah and his contemporaries that for a time, their patients embody the Canadian rock band The Sheepdogs’ jam, “I’ve Got A Hole Where My Heart Should Be” (it’s the unofficial heart transplant surgeon anthem, according to Shah). They are constantly pushing to keep people off the operating table and to save more lives when hearts break far away from medical centers.
“I am really focused on how do you resuscitate these hearts and recondition them? How do you get a heart that’s dysfunctional and make it better?
What are the therapeutics out there? What are the maneuvers that control the reperfusion? How do I operationalize what I know from a basic science standpoint works? How do we do that clinically? Whether it’s people who have a cardiac arrest in the street or whether it’s coaxing that heart transplant I did last night to work to the everyday heart operations that we do. I think about that a lot,” said Shah.
Tune in on your favorite platform: Apple Podcasts, Google Podcasts, Spotify, Stitcher, Pandora, and the Health Podcast Network.
Join the conversation on Twitter and LinkedIn with #ListenDNA and by following @VUMC_Insights.