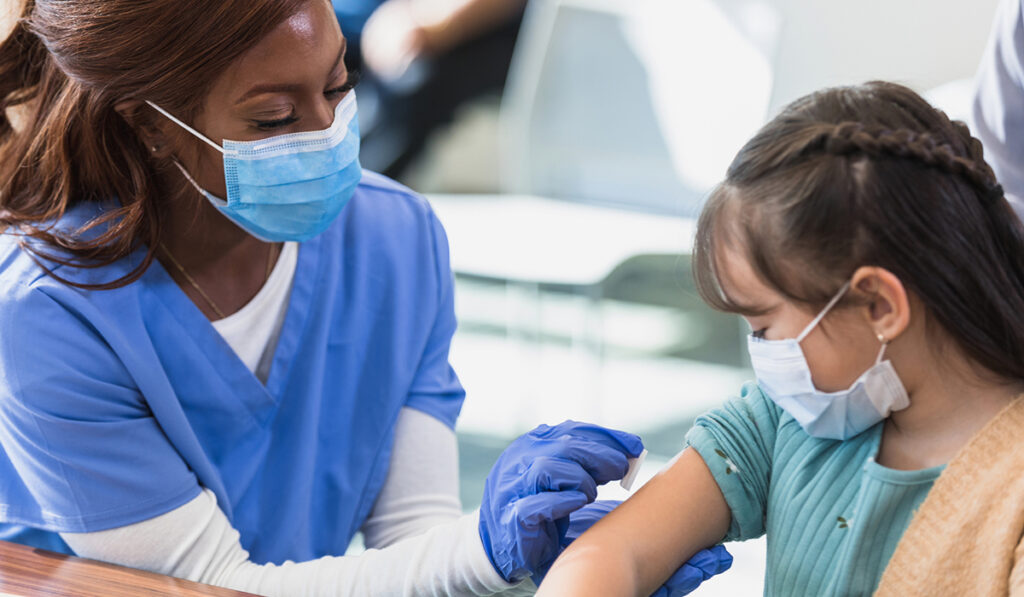
Research has shown that adult acceptance of the COVID-19 vaccine is influenced by myriad factors, including access to information, misinformation, and concerns about side effects.
Thus, it is essential for pediatricians, public officials, and those charged with implementing school strategies to understand parental attitudes and expectations surrounding the COVID-19 vaccine.
A team of researchers at Monroe Carell Jr. Children’s Hospital at Vanderbilt reported in a study published in Clinical Pediatrics that parents who are reluctant to vaccinate their children against influenza are more than five times as likely to decline the COVID-19 vaccine for their children.
The Vanderbilt Child Health Poll is conducted annually from a representative sample of Tennessee parents to capture data on the sociodemographic characteristics of families, overall health, and health-care equity. The survey gauges concern about a wide range of topics, including insurance status, child mental health, and food insecurity.
“We included additional questions to better evaluate perception and acceptance of COVID-19 and influenza vaccines to develop strategies going forward,” said Mia Letterie, lead author of the paper and associate program manager for the Vanderbilt Center for Child Health Policy.
“We assumed where people live, their education levels, race and other factors would have a higher impact on parental acceptance of COVID-19 vaccines in children.”
Acceptance of the flu vaccine, somewhat surprisingly, “was a primary determinant,” she added.
Demographic Differences
The 2021 survey was administered in late fall 2020, prior to the availability of COVID-19 vaccines. Data from 1,066 parents were analyzed using weighted survey methods to generalize results to the state of Tennessee.
Overall, more than half – 64 percent – of parents reported being likely to accept the influenza vaccine for their child, while 53 percent of parents reported being likely to have their children vaccinated against COVID-19. Yet only 45 percent of those surveyed said they were likely to vaccinate their child against both COVID-19 and influenza.
“This was a big takeaway for me,” Letterie noted.
Additional analysis revealed that parents who identified as Hispanic were 61 percent in favor of vaccinating their children against COVID-19 compared to 54 percent of non-Hispanic whites and 44 percent of non-Hispanic Black parents. However, the biggest revelation was in hesitancy difference by gender.
“Females were less accepting of the COVID vaccine than male parents, which was surprising,” said Elizabeth Williams, M.D., an assistant professor of pediatrics at Monroe Carell and an investigator on the study team. “We can’t explain the gender findings, but it tells us that additional studies are warranted.”
Masking and School Safety
The 2022 analysis of the Vanderbilt Child Health Poll looks at virus prevention efforts in schools, specifically masking and vaccines. The poll was conducted in late fall 2021, before the rise of the Omicron variant in Tennessee and revisions to prevention measures at some schools.
About 67 percent of 1,026 parents surveyed said their kids attend school with a mask on, and 53 percent said their child’s school has a mask requirement.
More than half of Black parents said they agreed that schoolteachers and staff should have to be vaccinated, while less than 40 percent of white parents and parents of other races and ethnicities agreed that school personnel should have mandatory vaccinations.
Regions of the state also have different opinions about vaccination requirements. More parents in Middle and West Tennessee, with higher concentrations of urban population, think school personnel should have to be vaccinated.
Improving Vaccine Education
Both surveys asked parents whom they trust to provide accurate information about the COVID-19 vaccines. In 2021, their child’s health care provider was described as the most trusted (42 percent) followed by the Centers for Disease Control (39 percent), medical research (34 percent) and the Tennessee Department of Health (31 percent).
Letterie says this is a trend they see continuing.
“Pediatricians should be talking with families and kids about the vaccines – taking time to answer questions, addressing any hesitancy and steering them to local resources as needed,” she added.
“Additionally, the poll highlights the need for public health organizations to focus on maximizing vaccine uptake for children. We know these vaccines are safe and that they work to prevent severe infection. It is essential that we communicate this to help increase COVID vaccination rates in children.”